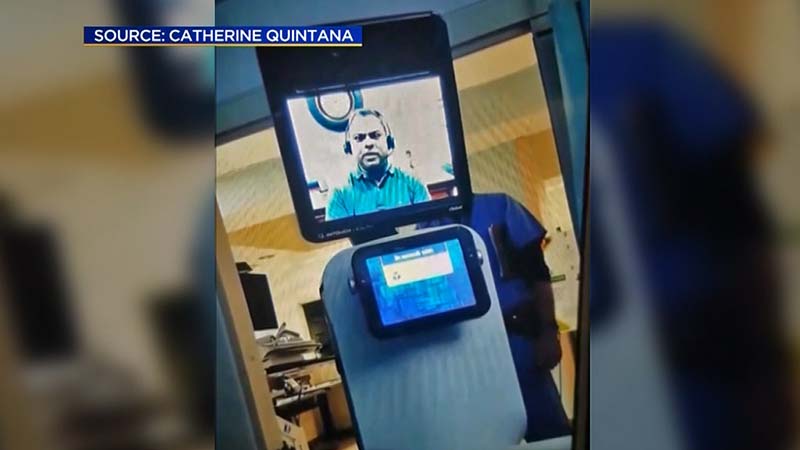
The video-screen carrying robot used by doctors to converse with patients.
The headline on the local news station’s website was sensational: “Bereaved Family Upset Kaiser Used Robot to Tell Father He Would Die”. Evoking some sort of post-modern dystopia, the article explains that the family “was taken by surprise when a robot rolled into the room” to deliver the news that an elder family member’s illness had progressed past the physician’s ability to treat it. While the robot actually was a remote physician using teleconferencing software to communicate with the patient and his family, the monitor projecting an image of the physician’s head and shoulders sat atop a tall, narrow metal unit reminiscent of a body. The “robot doctor” story was picked up by national news outlets, like the New York Times, and medical ethicists weighed in on the ethics of communicating “sensitive” topics remotely. The news stories problematized the impersonal, almost routinized, care as it was perceived by the family. In one, a representative from the American Medical Association commented, “We should all remember the power of touch – simple human contact – can communicate caring better than words.”
The “robot doctor” described above is part of an initiative to deliver medical care remotely via telehealth technologies. The American Medical Association has ethical guidelines for the practice of telehealth/telemedicine, which “involve care delivered to a patient at an originating (or spoke) site from a specialist working at a distant (or hub) site” (HRSA 2019). The AMA guidelines (2017)—for medical doctors who provide medical care remotely—acknowledge the limitations of telehealth technologies in diagnosis and in relationship-building with patients. An editorial published in the Journal of General Internal Medicine shortly after the release of the AMA’s guidelines cautions practitioners to remember: “The practice of medicine is inherently a moral activity, founded in a ‘covenant of trust’ between patient and physician” (Chaet et al 2017). Technology mediates the “moral activity” of medicine in a variety of ways, and some have argued that it generates an imperative to evaluate its use in the many contexts of health care (Bjorn 2002).
In our work, we have found that technologies mediate advance care planning and end-of-life conversations. For the past two years, we have been interviewing health care providers and people living with cancer to learn about their practices of, and perspectives on, advance care planning. Advance care planning refers to making decisions about one’s health care in advance of a situation in which they would not be able to express their wishes. Advance directive documents (e.g. do not resuscitate orders), as technologies that communicate a person’s wishes for medical care, can stand-in for patients’ conversations with providers about their end-of-life wishes. Tele- or video-conferences mediate end-of-life conversations between Spanish-speaking patients and their English-speaking physicians. Here, we focus on technologies of interpretation, and explore their use in a context that juxtaposes the (im)personal and technological by examining the technologies themselves and the ethical positions of providers toward those technologies.
What is ethical interpretation in the health care context?
Language interpreters[1] have long been present and made use of in business as the globalization of corporations required interactions in multiple languages. Remote language interpretation and translation businesses may fill the need for on-demand interpretation in hundreds of languages. The use of translators and interpreters for health care provider/patient communication includes written information and conversations about critical issues such as diagnoses, adherence to medications, test and exam results, and even end of life discussions and choices.
In our field site, patients with speech, visual, hearing, sensory or manual impairment or language barriers are offered interpretation services free-of-charge. While interpretation/translation by family, friends, or untrained staff members is prohibited, except in the cases of emergencies, non-certified persons may be relied upon until a staff or contracted (remote) medical interpreter is available. In the health system where we conducted interviews with providers, they contract with an interpretation company for remote services, particularly for less common languages. According to one interpretation contractor, all of their spoken language interpreters are certified or in the process of certification by national entities (e.g. the National Board of Certification for Medical Interpreters). The contracted services tout their interpreters around-the-clock availability and they guarantee confidentiality.
How is ethical interpretation produced during advance care planning/end-of-life conversations?
Despite interpretation companies’ guarantees of service availability 24-hours-a-day, 7 days-a-week, remote interpreters’ professionalization and the local availability of hardware may affect the quality and accessibility of interpretation. While telephone or video interpretation was available to the providers in our study, our interviewees reported shortcomings with remote interpretation (via telephone or video) during ACP conversations. One clinic staff member reported on an occasion when a phone interpreter could be heard doing dishes during an appointment, which the staff member felt was very unprofessional. Additionally, interpretation technology is not always readily available nor does it operate as intended. One provider reported that on her floor of the hospital, they have to share a handful of mobile video interpretation devices. This means that sometimes all are being used and it is time-consuming to track one down, which is not ideal for urgent situations. Another provider commented, “You have to dial in [to the phone interpretation service], the conversation cuts off. Sometimes we have the video monitors and it freezes. It just is a whole other set of barriers.”
Interacting with interpretation technology—both the hardware and the human—may take additional time. Furthermore, our study participants noted that ACP discussions often take longer than a normal clinic visit allows, and this time limitation is exacerbated when there is a need for interpretation. ACP conversations can require a physician to engage in a “process of managing information, particularly bad and uncertain news” (Clemente 2015). An oncologist who has practiced for more than a decade said that the sensitive nature of ACP makes it even trickier to use an interpreter: “…translation [sic], especially if I’m tired, it’s just—it becomes a stressful thing… you have to pull out a different way of thinking and speaking and it takes longer, and… it’s more concentration and tense, and it can be very draining in a situation that is already draining.” Not all primary care physicians (PCPs) and oncologists we interviewed had problems with remote interpretation services, but many felt that in-person interpretation is more reliable and, as one oncologist pointed out, it “shows more compassion” and is “more humane” than when technology facilitates the conversation. This preference for in-person interpretation, sometimes on both the part of the health care professional and the patient, may lead to family members being used as interpreters during the clinical encounter.
In conclusion, we would like to highlight the oncologist’s comment about in-person interpretation being “more humane” and the AMA spokesperson’s emphasis on the need for “simple human contact” in effective health care communication. Both suggest shared understandings about what it means to demonstrate care for patients, and express concerns about modes of human-to-human interaction that are modified by technologies. As others have pointed out (Norris et al 2005), language interpretation during end-of-life discussions requires complex interactions between members of the health care team and may necessitate preparation that would not be feasible in the case of contracted interpretation. In order to understand how patients, like the family described at the beginning of this post, feel about mediated discussions about ACP with their physicians, we are currently analyzing data from interviews with Spanish-speakers who have been through cancer treatment.
References Cited
Chaet, Danielle et al. “Ethical practice in Telehealth and Telemedicine.” Journal of general internal medicine vol. 32,10 (2017): 1136-1140. doi:10.1007/s11606-017-4082-2
Clemente, I. (2015). Uncertain Futures. Communication and Culture in Childhood Cancer Treatment. Oxford & New York: Wiley-Blackwell.
Health Resources and Services Administration. (2019) Telehealth Programs. https://www.hrsa.gov/rural-health/telehealth/index.html, accessed Aug 10, 2019.
Hofmann, Bjørn. 2002. “IS THERE A TECHNOLOGICAL IMPERATIVE IN HEALTH CARE?” International Journal of Technology Assessment in Health Care 18 (3). Cambridge University Press: 675–89.
Norris, Wendi M, Marjorie D Wenrich, Elizabeth L Nielsen, Patsy D Treece, J Carey Jackson, and J Randall Curtis. “Communication about End-of-life Care between Language-discordant Patients and Clinicians: Insights from Medical Interpreters.” Journal of Palliative Medicine 8, no. 5 (2005): 1016-1024.
[1] Interpretation refers to spoken language, whereas translation refers to written language.
