(Editor’s Note: This blog post is part of the Thematic Series Data Swarms Revisited)
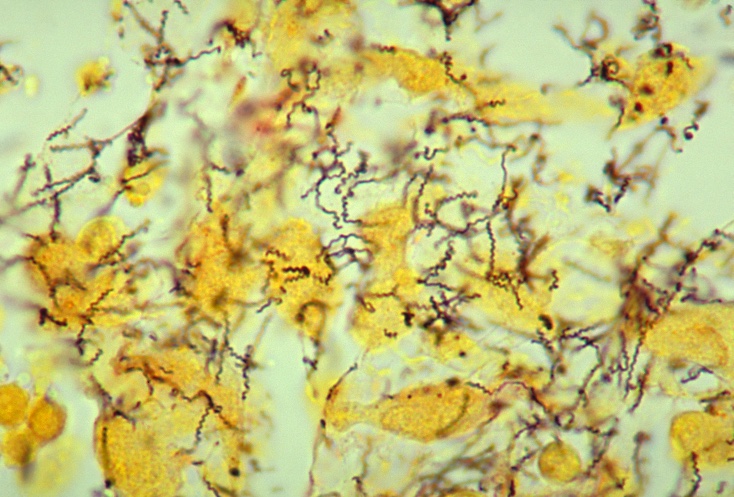
Treponema pallidum spirochetes under microscope using a modified Steiner silver stain. Obtained from the CDC Public Health Image Library. Image credit: CDC/Dr. Edwin P. Ewing, Jr, 1986.
Syphilis, an infection caused by the bacterium treponema pallidum, is an important disease. It starts as a skin lesion and develops until it deforms bones, compromises the central nervous system, and ultimately causes death. During pregnancy, the disease can also be transmitted from mother to child.
It has accompanied our species at least since the Renaissance and generated various innovations in modern science throughout this history. It helped give rise to serology through the Wasserman Reaction (Fleck 2010), the first detection test, and it was crucial for the consolidation of somatological perspectives of mental illnesses in psychiatry (Carrara and Carvalho 2010). Due to sexual transmission of the disease, in the eighteenth and nineteenth centuries, it became the evil venereal illness par excellence in restrictive sexual regimes (Fleck 2010; Quetel 1986). Since that time, syphilis has laid the foundations for codes of social conduct and even for ideas of the “self” in western societies, for example in criminalizing prostitution (Carrara 1996; Bastos 2007) and shaping contagion theories and its relations of body-subject (Echeverría 2010).
The advent and global distribution of penicillin after the 1940s, which is still the main therapy for syphilis, controlled the disease’s increase and prevented its more severe manifestations. However, nowadays syphilis is reemerging. In 2016 the WHO recognized, at the Sixty-ninth World Health Assembly, that penicillin was a drug in short supply on the global health market and that this causes an increase of syphilis in many countries (Brasil 2016). This is not just in countries of peripheral capitalism. According to a 2019 report by the European Center for Disease Prevention and Control, between 2010 and 2018, there was a 70 percent increase in syphilis notifications in Europe (ECDC 2019).
Here, I consider the epidemiological reality of syphilis in Brazil – where the disease is considered an epidemic since 2016[1] – towards developing some thoughts in the context of the Thematic Series on posthumanism and in relation to the cunning expression of “data swarms.” I focus specifically on the datafication process in the surveillance of syphilis, following Hacking’s proposal (1991) to analyze statistical thinking as a style of reasoning endowed with historical developments and effects on the framing of reality. I begin with some historical events amid the epidemiological quantification of syphilis, giving special attention to the invention of the notification category of “syphilis in pregnant women.”
I argue that the transformation of syphilis into epidemiological data creates a reality that claims a truth about the disease. This process involves the mutual implication of representations and interventions, and, as I show, these dimensions of modern sciences are both practices. In what follows, I reflect on issues such as: What does it mean to live between data and information? What are the conditions of possibility and the consequences of turning a phenomenon into a cluster of data? What are the effects of datafication and quantification for the ways in which a disease is understood and performed?
Epidemiological Quantification of Syphilis in the Brazilian Health System
In the 1980s in Brazil, there was no standardized and continuous data production available to measure the distribution and characteristics of syphilis. While some states registered only deaths, others included detected cases, or suspected cases were counted in addition to those confirmed. There were also occasional studies, which covered health services, municipalities, neighborhoods, states, regions of the country or of national inference via estimates.
At that time, it was understood that congenital syphilis was on the way to its eradication, a project over which an “optimistic environment” hovered (Lima 2002: 268). This scenario was based on syphilis mortality rates, which decreased by 5 percent from 2.45 to 1.02 per one million inhabitants between 1980 and 1995.
It was in this context that, in 1986, congenital syphilis was instituted as a notifiable disease in Brazil. It became imperative that the cases detected by the assistance services were also sent to the surveillance agencies by means of forms that were dutifully filled out. This was an important mechanism for consolidating the Brazilian health system, which was being reformulated toward a free, universal, and state-financed system. This was formally constituted in 1988, in the midst of the re-democratization process that unfolded after twenty-five years of civil-military dictatorship.
Mandatory notification was essential for establishing a consensus on what to account for in cases of congenital syphilis and how this should be done: What is necessary to be recorded? What criteria are valid for confirming cases? When does notification have to be made and what is the institutionalized and bureaucratic flow of recorded data?
However, the institution of the mandatory notification did not immediately result in the production of national indicators. For this, it was necessary to create the National System of Notifiable Diseases in 1993. This is the informational environment that gathers and transforms the notified cases in coefficients and rates. It was only in 1998 that instruments were developed, information flows were defined, and software for the system was developed, which standardized the sending of notification forms to the surveillance agencies.
In 2004, another event enhanced the epidemiological visibility of syphilis. The Pan American Health Organization launched a project to entirely eliminate its vertical transmission for Latin America and the Caribbean region. This program had an important effect in giving a prominent position to the disease within the health policies of Brazil. The elimination of syphilis’s vertical transmission was included as the top priority in the 2004 Ministry of Health’s National STD-AIDS Program. Notification data for congenital syphilis started to be published in epidemiological bulletins. The case definition for congenital syphilis was also reformulated and the category of notification “syphilis in pregnant women” was instituted. This notification category went on to play an important role in the quantification of syphilis.
Syphilis in Pregnant Women
In 2005, the cases for pregnant women with syphilis were low (at 1.863 cases) when compared with the number estimated by a prevalence study held by the Ministry of Health a year before (at 48.425 cases). Underreporting was calculated by the following operation: the difference between the number of notified and estimated cases. It is for this reason that a rise of more than 400 percent in the reported cases over the next five years (2010 registered 10.084 cases and a rate of 2.4 in one thousand live births), was not considered enough for syphilis to be an epidemic. This rise just unveiled a reality that was underreported.
In 2016, the rate of syphilis in pregnant women was 13.4 in one thousand live births, increasing again by more than 400 percent. At this moment, syphilis was already considered an epidemic in Brazil, and therefore the numbers were taken as reality. This implied a change in the calculations to tackle underreporting: now it was determined by the difference between the rates of “syphilis in pregnant women” and “congenital syphilis.” The state-run Epidemiological Bulletin claimed that the Brazilian states of Alagoas, Ceará, Pernambuco, Piauí, Rio Grande do Norte, Sergipe, and Tocantins “presented rates of congenital syphilis higher than those of syphilis in pregnant women, which refers to possible gaps in the epidemiological surveillance system” (Brasil 2016: 4).
The difference between the rates of syphilis in pregnant women and congenital syphilis indicated underreporting because every child born with syphilis acquired the disease from the mother. Thus, with more notifications for newborns than pregnant women, there is underreporting in the latter category. The comparison is possible because the calculation of these two indicators is formed by the same denominator: the total number of live births of mothers living in the same place and in the same year, and both are multiplied by the same factor of one thousand.
In 2018, the Ministry of Health noted an “improvement in the notification of syphilis in pregnant women” (Brasil 2018: 8), since four states registered rates for this category higher than those of congenital syphilis. This left just two states, Pernambuco and Rio Grande do Norte, still showing the opposite. In the following year, the expansion of syphilis detection tests and prenatal care networks, as well as the promotion of training courses for health professionals on notification procedures, were implemented to improve the registration of cases. By 2019, it was reported that “no Federation Unit had a higher incidence rate of congenital syphilis than the detection rate of syphilis in pregnant women” (Brasil 2019: 9).
Syphilis as Data Swarm
Syphilis monitoring constitutes a scaling question. It is possible to determine its distribution and characteristics in different spatial and temporal sections: between cities and states, in the national territory for different historical periods, and even on an international scale. This is a way to claim both a truth and (ac)countability for the disease.
The notification category “syphilis in pregnant women” had an important effect in consolidating syphilis as an epidemiological reality. It established a self-referential verification method, the identification of the underreporting by the difference between its rates and those of congenital syphilis. The parameter for this calculation is no longer external to the notification process, as was the prevalence study.
More than merely a detection technique, this operation sets criteria for understanding the disease that makes it visible, quantifiable, and also subject to intervention. For example, measures of improvement for the surveillance system were held when rates of syphilis in pregnant women were lower than those of congenital syphilis.
Translating syphilis into a data swarm is not only a way of representing but also of intervening, since the data is the production of a reality for interference: representation and intervention are in a relation of mutual implication. Information and control operate a medicine that transforms the infected body into a code – a health indicator – that distributes life in numbers. Following Deleuze, this is a medicine
“without doctor or patient” that singles out potential sick people and subjects at risk, which in no way attests to individuation – as they say – but substitutes for the individual or numerical body the code of a “dividual” material to be controlled (Deleuze 1992: 7).
We are used to thinking that interventions are concrete practices. The datafication process of syphilis shows us that representations are practices too, which offers a way to think about the politics involved. These epidemiological visibilities emerge through protocols that are “technoscientific rules and standards that govern relationships within networks” (Galloway and Thacker 2007: 28). Notification forms, case definitions, detection tests, and epidemic protocols materialize decisions about how to translate a biological life – a bacteria that infects a body – into a set of data: a reality susceptible to interference. They are condensed biopolitics.
Acknowledgments
I am very grateful for the contributions of Christoph Lange and Marcello Múscari. My thanks also to Serena Stein for her editorial assistance.
Read more of the Data Swarms Series:
Data Swarms Revisited – New Modes of Being by Christoph Lange
Human as the Ultimate Authority in Control by Anna Lukina
Angelology and Technoscience by Massimiliano Simons
Multiple Modes of Being Human by Johannes Schick
On Drones and Ectoplasms: Breath of Gaia by Angeliki Malakasioti
Fetishes or Cyborgs? Religion as technology in the Afro-Atlantic space by Giovanna Capponi
Notes
[1] See https://saude.estadao.com.br/noticias/geral,ministro-da-saude-admite-que-brasil-vive-uma-epidemia-de-sifilis,10000083382 [last access on 07/06/2021].
References
Brasil 2016. Ministério da Saúde. SÍFILIS. Boletim epidemiológico, Brasília.Brasil 2019. Ministério da Saúde. SÍFILIS. Boletim epidemiológico, Brasília.Carrara, Sérgio; Carvalho, Marcos 2010. A sífilis e o aggiornamento do organicismo na psiquiatria brasileira: notas a uma lição d doutor Ulysses Vianna. História, Ciência. Saúde-Manguinhos, Rio de Janeiro, v. 17.Deleuze, Gilles 1992. “Postscript on the Societies of Control.” October, vol. 59, 3–7.Echeverria, Virginia 2010. “Girolamo Fracastoro and the Invention of Syphilis.” História, Ciência, Saúde-Manguinhos, Rio de Janeiro, v.17, n.4, 877–884.ECDC – European Centre for Disease Prevention and Control 2019. Syphilis and Congenital Syphilis in Europe – A Review of Epidemiological Trends (2007–2018) and Options for Response. Stockholm: ECDC.Fleck, Ludwik 2010. Gênese e desenvolvimento de um fato científico. Tradução, Georg Otte, Mariana Oliveira. Belo Horizonte: Fabrefactum.Galloway, Alexander R.; Thacker 2007. The Exploit: A Theory of Networks. Minneapolis: University of Minnesota Press.Hacking, Ian 1991. “How should we do the history of statistic?” In: Burchel, G.; Gordon, C.; Miller, P. (eds.), The Foucault Effect: Studies in Governmentality. Chicago: The University of Chicago.Lima, Bruno Gil 2002. Mortalidade por sífilis nas regiões brasileiras, 1980-1995. Jornal Brasileiro de Patologia e Medicina Laboratorial, v.38, n.4, 267–271.Quétel, C 1986. Le mal de Naples: histoire de la syphilis. Paris: Seghers.

1 Trackback